You wake up already tired.
Nothing obvious is wrong, but your patience is shorter, your energy feels uneven, and everything feels harder than it should. You still have to get everyone out the door: the kids need breakfast. Work starts in an hour. Your partner somehow slept through the chaos. Your body feels like it’s running behind.
You check your calendar and realize it’s that time of the month. There’s a strange comfort in having an explanation. You know why your body feels a little less steady, and there’s reassurance that it will pass. That predictability adds to your resilience.
These shifts are often explained as hormonal, but hormones don’t act alone.
Behind the scenes, there’s a deeper regulator quietly shaping how the body responds, adapts, and recovers: the vagus nerve.
What Is the Vagus Nerve? Your Body's Hidden Stress Regulator
The vagus nerve is the central communication highway between your brain and body. It continuously tracks your internal state—heart rate, inflammation, digestion, and even emotional tone—and helps maintain inner balance.
Think of it like a biological dimmer switch. The vagus nerve does not just turn stress “on” or “off.” It adjusts how strongly your body reacts, how long a response lasts, and how efficiently you recover.
When vagal tone is strong, stress responses tend to feel more manageable, recovery is more efficient, and emotional regulation feels easier. When vagal tone is reduced, stress can feel amplified, recovery often slows, and systems like sleep, mood, and digestion become less predictable.
For women, this system is closely intertwined with hormonal fluctuations, and its effects can shift across different stages of life.
The Menstrual Cycle and Your Nervous System: Why Stress Hits Harder Before Your Period
Cyclical Stress, Emotional Sensitivity, and Recovery
Starting at puberty, women experience reproductive years marked by monthly hormonal rhythms—particularly shifts in estrogen and progesterone—that create predictable changes in physiology.
But what often gets overlooked is how these hormonal cycles interact with the autonomic nervous system. For many women, this interaction is what makes pre-menstrual syndrome (aka. PMS) feel more than just a mood shift.1 And for some women, conditions like menstrual migraine, endometriosis, or PCOS can be triggered and feel especially disruptive during certain phases of the cycle.
What’s happening beneath the surface
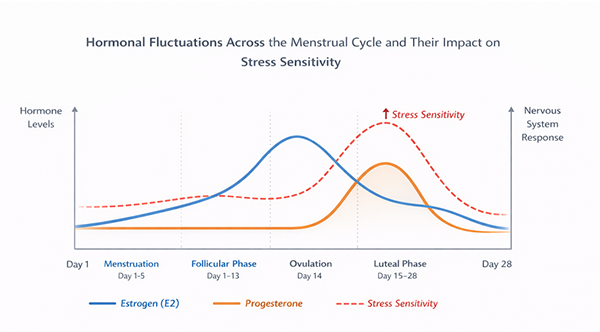
In the days leading up to menstruation (the luteal phase), progesterone rises and then falls. As these hormone levels shift, sensitivity to stress often increases, and heart rate variability, a marker of vagal tone, may decrease.1
Together, these changes can make the system more reactive and slower to recover, especially for women already navigating cyclical pain, inflammation, or hormone-related symptoms.
 What this often feels like is subtle but significant: more irritability, a shorter fuse, a lower threshold for overwhelm, or a level of fatigue that doesn’t quite match how much rest you got. The same stressors that felt manageable two weeks earlier can suddenly feel heavy.
What this often feels like is subtle but significant: more irritability, a shorter fuse, a lower threshold for overwhelm, or a level of fatigue that doesn’t quite match how much rest you got. The same stressors that felt manageable two weeks earlier can suddenly feel heavy.
This is where resilience becomes more than a mindset. It reflects how efficiently your body can absorb stress, regulate it, and return to baseline. During certain phases of the menstrual cycle, that recovery buffer may be naturally reduced.
A helpful way to think about it: hormones set the “weather,” but the vagus nerve determines how well you tolerate the storm.
Where non-invasive vagus nerve stimulation (nVNS) may help
nVNS provides a way to gently support these regulatory circuits during times when the body may feel more reactive. By activating vagal pathways, it can help shift the nervous system toward a more parasympathetic, recovery-oriented state, making stress responses feel less exaggerated and helping the body reset more efficiently after emotional or physical strain.
Rather than suppressing symptoms or overriding hormonal changes, this approach helps the nervous system respond to physical and emotional demands in real time. In the context of the menstrual cycle, that may mean feeling less depleted by normal daily demands and better able to maintain a greater sense of stability day to day.
Why Everything Feels Harder in Perimenopause: A Nervous System Explanation
Variability, Unpredictability, and Nervous System Load
Perimenopause is often described as a hormonal rollercoaster, but the lived experience is usually less about intensity and more about unpredictability.
During perimenopause, cycles become irregular. Estrogen can rise and fall dramatically. Sleep often becomes more fragmented. And over time, the body loses some of the consistency it once relied on.
One of the most frustrating parts of this stage is that the same routines, habits, or coping strategies that once worked may suddenly feel less effective. A stressful meeting, a poor night of sleep, or a small disruption in routine can feel disproportionately destabilizing.
What changes physiologically
During perimenopause, shifting estrogen levels begin to influence brain regions involved in autonomic regulation. Thermoregulation becomes less stable, contributing to hot flashes and temperature sensitivity, while sleep architecture often becomes more fragile. Together, these changes increase variability across systems that are typically more tightly regulated.
This is why women in perimenopause may experience sudden anxiety, panic-like sensations, frequent night awakenings, or a growing sensitivity to stressors that once felt manageable. The system is still working, but it’s operating with less predictability and less reserve.
This matters because resilience during perimenopause is not just about tolerating change. It’s about how efficiently the nervous system can recalibrate after disruption. When hormonal signals become less consistent, that recalibration process can feel slower and less reliable.
A helpful way to think about this stage: the system is still functional, but the internal signals have become noisier. This makes it harder to find and maintain equilibrium.
The role of vagal regulation in perimenopause
The vagus nerve plays a central role in supporting stability during this phase by helping regulate heart rate, facilitating transitions into and out of sleep, and modulating inflammation and stress signaling.
When vagal tone is supported, physiological swings may feel less extreme, recovery between stressors can become more efficient, and sleep onset and continuity may improve.2
In this context, nVNS offers a targeted way to reinforce these regulatory pathways. It may help the system regain some consistency even amid ongoing hormonal variability. Rather than changing the inputs, it supports how the body regulates them, which can help restore some of the consistency the body relies on.
Menopause and Vagal Tone: When the Body Feels Calm But Less Resilient
Stability Without Flexibility
After menopause, hormone levels become more stable, but at a lower baseline. This loss of estrogen matters because it plays an important role in autonomic regulation, metabolic function, and neural signaling.3
So while the unpredictability of perimenopause often settles, a different challenge can emerge: the body may feel steadier, but it’s less buffered. It is no longer navigating dramatic monthly swings, yet its ability to adapt and recover from stress can become less efficient over time.
What shifts physiologically
With lower estrogen levels, baseline parasympathetic activity may decrease and inflammatory signaling can increase. Together, these changes can reduce the body’s ability to absorb stress and recalibrate after strain.
For many women, this shows up less dramatically than perimenopause, but more persistent: fatigue that lingers, a lower tolerance for daily stressors, or a slower recovery after emotional or physical strain.3 In this stage, the challenge is often less about fluctuation and more about diminished physiological reserve.
In menopause, resilience looks a little different. The goal is no longer simply getting through unpredictable swings. It’s about maintaining the flexibility and recovery capacity that support long-term well-being.
A helpful way to think about this stage: the system may feel calmer on the surface, but it has less built-in cushion when demands increase.
Supporting long-term nervous system regulation with nVNS
nVNS may help support the regulatory systems that become increasingly important during this phase. Research suggests it can influence pathways involved in autonomic balance, neuroinflammatory signaling, mood, and cognitive function. These are areas that all contribute to how resilient the body feels over time.
Clinical observations in neurological populations have shown improvements across cognitive, emotional, and physical symptoms with nVNS use, highlighting its role in broad system regulation rather than single-symptom targeting.4
While menopause is not a disease state, many of the same core regulatory pathways remain relevant. In this stage, the goal is less about correcting a deficit and more about supporting the body’s capacity to adapt. Rather than targeting one symptom at a time, nVNS may help maintain the steadiness, flexibility, and long-term adaptability that supports resilience.
nVNS is safe to use in your daily life, and it is important to choose devices that are clinically proven, like Truvaga. The right device, placement and consistent daily use can help you sleep better, feel calmer and more focused.
The Vagus Nerve Across All Life Stages: A Whole-Body View of Resilience
Across menstruation, perimenopause, and menopause, the underlying theme is not just hormonal change, but how the nervous system responds to it.
At every stage, the vagus nerve helps shape resilience by buffering stress, supporting stability during periods of change, and helping the body recover more efficiently after strain.
If hormones are the signals, the vagus nerve helps determine how those signals are processed, integrated, and ultimately experienced. In that sense, supporting vagal tone is less about chasing symptoms and more about strengthening the mechanisms that helps women adapt, recover, and stay resilient across every phase of life.
5 Evidence-Backed Ways to Strengthen Your Vagus Nerve Daily
While technologies like nVNS provide targeted support, everyday practices can also reinforce vagal function:
- Slow, Controlled Breathing
Aim for longer exhales than inhales
→ Signals safety to the nervous system and supports parasympathetic activation - Cold Exposure (Brief and Gentle)
Splashing cold water on the face
→ Activates vagal reflex pathways and can help reset stress responses - Consistent Sleep Timing
Regular sleep-wake cycles stabilize autonomic rhythms
→ Supports recovery, especially during hormonally sensitive phases - Social Connection
Positive interactions stimulate vagal pathways linked to emotional regulation
→ Reinforces resilience through co-regulation - Non-Invasive Vagus Nerve Stimulation (nVNS)
Provides direct, reproducible activation of vagal circuits
→ Especially useful during periods of heightened stress, hormonal transition, or reduced recovery capacity
Final Takeaway
A woman’s physiology is not static. It evolves across decades.
What often feels like hormonal chaos is, in many cases, a reflection of how well the nervous system is able to regulate change.
By supporting the vagus nerve, you’re not chasing symptoms. You are strengthening the system that determines how your body responds, adapts, and recovers.
And ultimately, that’s what resilience is: not avoiding stress, but having the capacity to move through it and return to balance at every stage of life.
Frequently Asked Questions (FAQs)
1. How does the vagus nerve affect women’s resilience?
The vagus nerve plays a central role in how the body responds to stress, recovers, and maintains emotional balance. In women, this becomes especially important because hormonal fluctuations—across the menstrual cycle, perimenopause, and menopause—can influence how reactive or sensitive the nervous system feels. Strong vagal tone helps buffer these changes, supporting adaptability, recovery, and overall resilience.
2. Can vagus nerve stimulation help with PMS or menstrual symptoms?
Non-invasive vagus nerve stimulation (nVNS) may help support the autonomic nervous system during the menstrual cycle. While it is not a treatment for PMS or menstrual conditions, it may help the body respond more efficiently to physical and emotional stress, which can influence symptoms like irritability, fatigue, and emotional reactivity. The goal is not to eliminate the effects of hormonal changes, but to improve how the body processes them.
3. Why does stress feel worse during perimenopause?
During perimenopause, hormone levels—especially estrogen—can fluctuate unpredictably. These changes may affect brain regions involved in stress regulation, sleep, and autonomic balance, making the nervous system more sensitive to everyday stressors. As a result, women may experience heightened anxiety, sleep disruption, or emotional variability. Supporting vagal tone during this phase may help improve recovery and support greater day-to-day steadiness.
4. Is vagus nerve stimulation safe for menopause-related symptoms?
nVNS is generally considered safe and well tolerated when used as directed. Emerging research suggests it may influence pathways involved in mood, inflammation, and autonomic balance—all of which are relevant during menopause. However, it should be used as part of a broader wellness approach and not as a replacement for individualized medical care.
References:
- Hamidovic A, Davis J, Soumare F, Naveed A, Ghani Y, Semiz S, Khalil D, Wardle M. Allopregnanolone Is Associated with a Stress-Induced Reduction of Heart Rate Variability in Premenstrual Dysphoric Disorder. J Clin Med. 2023 Feb 16;12(4):1553. doi: 10.3390/jcm12041553. PMID: 36836088; PMCID: PMC9967763.
- Grillot JM, Staats PS (2025) An Open-Label Trial of Cervical Non-Invasive Vagus Nerve Stimulation Using a Proprietary Signal for the Management of Sleep and Depressed Mood. JSM Anxiety Depress 6(1): 1029
- Santoro N, Roeca C, Peters BA, Neal-Perry G. The Menopause Transition: Signs, Symptoms, and Management Options. J Clin Endocrinol Metab. 2021 Jan 1;106(1):1-15. doi: 10.1210/clinem/dgaa764. PMID: 33095879.
- Ament M, Leonard E, Staats PS, Ingram NT. Retrospective post-hoc subgroup analysis of adjunctive non-invasive vagus nerve stimulation in chronic mTBI with comorbid PTSD. Front Neurol. 2026 In Press
Author bio:

 US
US  UK
UK 





